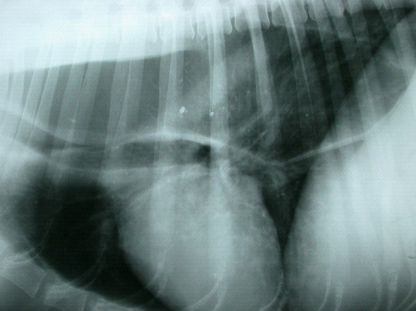
WHAT ARE THE ADRENAL GLANDS?
The adrenal glands are two small bean-shaped organs less than 1cm in height and width that are located next to each kidney in the abdomen. They produce several hormones, two of which are crucial for survival. These are glucocorticoids (cortisol) and mineralocorticoids (aldosterone). Glucocorticoids have many functions in ensuring you feel well. Cortisol is important for responding to stress. It also helps stimulate appetite, affects immune function and maintains a normal blood glucose. The main mineralocorticoid, aldosterone, is important for salt (electrolyte) concentrations in the body fluids, specifically sodium and potassium. Too much or too little of either glucocorticoids or mineralocorticoids causes serious medical problems.
WHAT IS HYPOADRENOCORTICISM?
Hypoadrenocorticism, also known as Addison’s disease, is sometimes called the great pretender as it can imitate all sorts of other diseases and therefore can be challenging to diagnose. This disease occurs when the adrenal glands produce too little of these important hormones (cortisol and aldosterone). In dogs and cats, it most often occurs when the body's own immune system attacks cells of the adrenal gland. The function of the immune system is normally to protect the body against foreign substances and organisms. In immune mediated disease the cells of the immune system cannot recognise 'self' from 'foreign’ and start attacking cells from the individual's own body.
CLINICAL SIGNS
WHAT ARE THE SYMPTOMS OF HYPOADRENOCORTICISM?
Hypoadrenocorticism is uncommon in dogs and rare in cats. Dogs most often affected are young to middle-aged of any breed, however in some breeds it may be hereditary (Standard Poodle, Bearded Collie). Animals that have hypoadrenocorticism commonly lose their appetite, have vomiting or diarrhoea and they become lethargic and weak. Animals may have chronic waxing and waning clinical signs over a period of months or may present in a crisis, critically unwell and in shock.
&geometry(278x56))